Congenital cytomegalovirus (CMV) infection can cause serious complications such as hearing difficulties and mental retardation in affected infants. A Japanese research team has discovered a new method for predicting congenital CMV infection during the prenatal period. This method is safe for both mothers and fetuses, and could potentially be adopted for general use. The findings were published on October 20 in the online version of Clinical Infectious Diseases.
Research team members include Professor YAMADA Hideto (Kobe University Graduate School of Medicine, Department of Obstetrics and Gynecology), Associate Professor TANIMURA Kenji (Kobe University Hospital Center for Perinatal Care), Project Professor MORIOKA Ichiro (Graduate School of Medicine, Department of Pediatrics) and Doctor MINEMATSU Toshio (Director of the Aisenkai Nichinan Hospital Research Center for Disease Control).
In the United States over 8000 children a year suffer from the long-term complications of congenital CMV infection, and the annual costs of caring for these children are estimated at 1-2 billion dollars. In recent years, some doctors have successfully combated these problems by using antiviral agents to treat infants with congenital CMV infection. To facilitate this, early diagnosis is vital. However, tests to identify the infection in infants (PCR tests that detect virus DNA in infants’ urine) are not widely carried out, and would incur huge financial costs if they were carried out for all infants. Currently the most realistic and financially viable approach is targeting pregnant women who have a high risk of congenital infection and testing their newborn infants with a PCR urine examination.
As shown in figure 1, congenital infection usually occurs when women who lack antibodies for CMV contract the virus for the first time during pregnancy (primary CMV infection). Pregnant women at high risk for congenital infection are generally identified by testing for the CMV antibody immunoglobulin M (IgM). There are often cases of women who test positive for CMV IgM antibodies during pregnancy, but in some cases tests remain positive for CMV IgM for several years after primary infection, which may cause pregnant women and their family undue worry. The most accurate method for detecting fetal infection during pregnancy is testing for viral DNA in amniotic fluid. However, the amniotic fluid sampling is an invasive procedure that can result in rupture of the membranes, uterine infection, or miscarriage. The research team looked for a non-invasive method of predicting congenital CMV in fetuses.
They surveyed 300 pregnant women who tested positive for CMV antibodies (IgM) and were classified as high-risk for congenital injection. They carried out clinical interviews, blood tests, ultrasounds, and DNA PCR tests for CMV using samples of the subjects’ blood, urine and uterine cervical secretion. The medical interviews tested whether the women had cold-like symptoms, the blood test included measuring white blood cell count, viral antigens, and an IgG activity test (to determine whether subjects had recent CMV infection), and the ultrasound examinations looking for symptoms of congenital CMV infection in the fetus. They also tested the women’s blood, urine and uterine cervical secretion for CMV DNA.
After statistical analysis of all the results, the team determined that fetal abnormalities revealed through ultrasound and positive PCR results for uterine cervical secretion were the two most effective ways to predict congenital infection before birth. This is the first report to demonstrate that uterine cervical secretion can be used to predict congenital CMV infection.
Both ultrasound and PCR tests for uterine cervical secretion are non-invasive procedures, and using them can offer a safer method to test high-risk pregnant women and predict the occurrence of congenital infection. Accurately identifying the affected infants enables doctors to start antiviral treatment early, and could improve the neurological prognosis of infants infected by CMV.
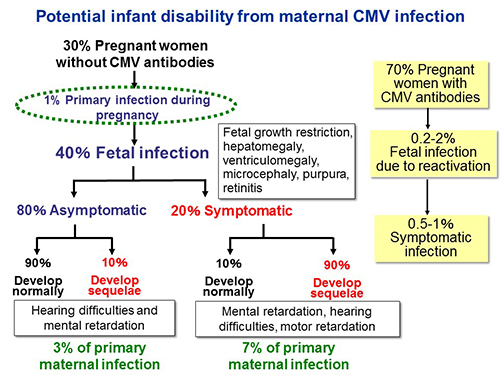
30% of pregnant women do not have CMV antibodies. 1% of this group will contract CMV for the first time during pregnancy. Among them, 40% of women will have viral transmission to fetuses. Even if the fetus contracts the virus, the infant will not necessarily suffer subsequent complications. One-fifth of infected infants are born with apparent symptoms, and 90% of this group will have sequelae. 80% of infected infants will not have apparent symptoms, but one-tenth of this group develop sequelae. Even if the woman has CMV antibodies before pregnancy, there is a low incidence of the virus reactivating and affecting the fetus.
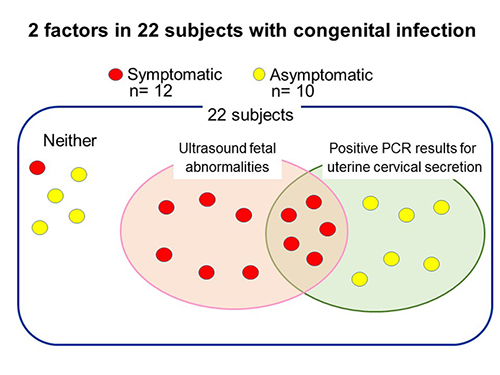
The red circles represent infants with apparent symptoms of congenital infection (symptomatic infection), and yellow circles represent infected infants without apparent symptoms (asymptomatic infection). Of 22 subjects with congenital infection, 11 with ultrasound fetal abnormalities were symptomatic. 11 subjects tested positive in PCR tests for the uterine cervical secretions, and 6 of them had no ultrasound findings were all asymptomatic. For 5 subjects with congenital infection had neither ultrasound findings nor positive PCR results, so caution is necessary.
Journal information
- Title
- “Prediction of congenital cytomegalovirus infection in high-risk pregnant women”
- DOI
- 10.1093/cid/ciw707
- Authors
- Kenji Tanimura, Shinya Tairaku, Yasuhiko Ebina, Ichiro Morioka, Satoshi Nagamata, Kana Deguchi, Mayumi Morizane, Masashi Deguchi, Toshio Minematsu, and Hideto Yamada
- Journal
- Clinical Infectious Diseases