A research group led by Kobe University Professor MORIOKA Ichiro (Graduate School of Medicine, Department of Pediatrics), Associate Professor OSAWA Kayo (Graduate School of Health Sciences, Department of Biophysics), and Clinical Technologist SATO Itsuko (Kobe University Hospital, Department of Clinical Laboratory) is proposing a new criterion for diagnosis of bacterial infection in preterm infants. Using this method could lead to early diagnosis and treatment for bacterial infection and improve the prognosis for preterm infants. These findings will be published in the online version of the journal Scientific Reports on April 1, 2016.
Infants born prematurely do not have fully developed immune functions. Compared to full-term infants, if preterm infants suffer a bacterial infection there is a higher chance of fatality or negative impact on future growth and development. However, in the case of preterm infants, it can sometimes be hard to detect the signs of bacterial infection visible in adults and other infants: fever, white blood cell count, and increase in C-reactive protein (CRP). An alternative method was needed to detect infection.
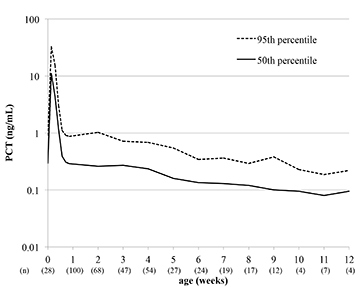
Professor Morioka’s research group focused on monitoring serum concentrations of procalcitonin (PCT), a marker used for early detection of bacterial infection in adults and children. Between June and December 2014, they examined 1267 serums from 283 newborns at the neonatal intensive care unit in Kobe University Hospital. The results demonstrated that PCT levels in full-term infants rose temporarily 1 day after birth, returning to the normal level for adults within 5 days (0.1ng/mL). However, for preterm infants it took 9 days after birth for PCT to return to normal levels.
Based on these results, the group plotted two reference curves: 50th percentile and 90th percentile values. When they superimposed 3 cases of preterm infants with bacterial infection on these curves, it clearly showed that in all three cases the serum PCT concentrations were higher than the 95th percentile values.
Use of this new criterion for detection of bacterial infection in preterm infants could help to improve their prognosis. “We could also potentially use this method to limit unnecessary use of antibacterial agents” commented Professor Morioka. “Our next step is to verify the precision of diagnoses based on these reference curves.”
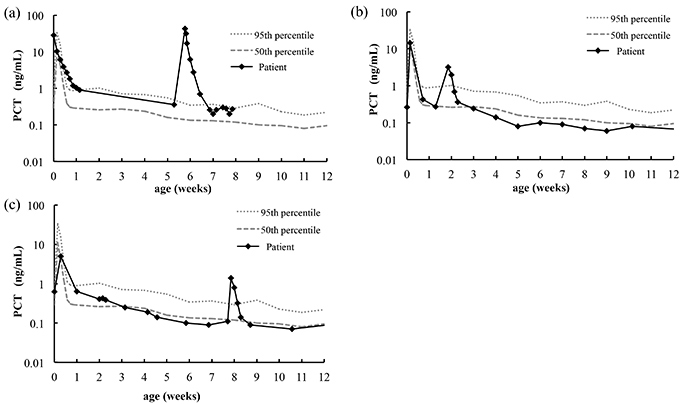
(a) A Japanese infant weighing 482 g was born at 22 weeks. At 42 days old, dyschromia and hypotension appeared. Enterobacter cloacae was detected from the blood culture. This case was diagnosed with culture-proven sepsis.
(b) A Japanese infant weighing 1,014 g was born at 27 weeks. At 12 days old, the infant was extubated; however, an apnea attack occurred. Chest radiography showed infiltration in the lung field. Pseudomonas aeruginosa was detected from the tracheal tube culture. This case was diagnosed with ventilator-associated pneumonia.
(c) A Japanese infant weighing 1,546 g was born at 30 weeks. At 55 days old, an apnea attack occurred. As no bacteria were detected from the blood culture, this case was diagnosed with clinical sepsis based on patient condition.
Journal information
- Title
- “Age-specific percentile-based reference curve of serum procalcitonin concentrations in Japanese preterm infants”
- DOI
- 10.1038/srep23871
- Authors
- Noriko Fukuzumi, Kayo Osawa, Itsuko Sato, Sota Iwatani, Ruri Ishino, Nobuhide Hayashi, Kazumoto Iijima, Jun Saegusa & Ichiro Morioka
- Journal
- Scientific Reports